Diabetes, chronic kidney disease, and British food culture
The prevalence of diabetes around the world has reached epidemic proportions. The International Diabetes Federation estimated that 537 million people were living with diabetes in 2021. This number is expected to increase to 784 million by 2045.
It has been estimated that 40% or more of people with diabetes will develop chronic kidney disease (CKD), including a significant number who will develop kidney failure requiring dialysis or transplantation. These are scary statistics, however the good news is so much can be done from a diet and lifestyle perspective to reduce the risk.
What is chronic kidney disease (CKD)?
It's a common condition often associated with getting older. It can affect anyone, but it's more common in people who are black or of south Asian origin. Also, conditions like diabetes, high cholesterol and high blood pressure put us at a higher risk of CKD.
The stages of CKD are based on how well your kidneys are able to filter out waste from your blood. The stages range from very mild (Stage 1) to kidney failure (Stage 5).
- Stage 1 CKD: Mild kidney damage, eGFR 90 or higher. Your eGFR is above 90ml/min (normal) but some other tests suggest you may have some kidney damage – for example, you have protein in your wee.
- Stage 2 CKD: Mild loss of kidney function, eGFR 60-89.
- Stage 3a & 3b CKD: Mild to severe loss of kidney function, eGFR 30-59.
- Stage 4 CKD: Severe loss of kidney function, eGFR 15-29.
- Stage 5 CKD: Kidney failure or close to failure, eGFR less than 15.
Scientific studies show that if recognised early, CKD in diabetes can be effectively slowed down. Diet and lifestyle play a fundamental part. Almost 1 in 5 people with diabetes will need treatment for diabetic nephropathy. Diabetes unfortunately remains the single most common cause of kidney failure in the UK.
One of the best ways to help prevent CKD or control it is to have as good as possible blood glucose control. One of the most common blood glucose tests is called HbA1c. Having a HbA1c of 48mmol/mol or less is associated with lower diabetes complication risk. HbA1c looks at the glucose attached to our red blood cells. Red blood cells live for 8-12 weeks, therefore a HbA1c can tell us what our levels have been for up to a 3-month period.

Diabetes nephropathy
High blood glucose levels cause extra blood to flow through the tiny filters in your kidneys, so they have to work harder than normal to clear it. Over time this can damage the filters, causing them to leak.
Renovascular disease
Diabetes and elevated blood pressure are risk factors for renovascular disease as they both cause a ‘furring’ of the artery to the kidney, reducing the blood supply and causing scarring.
What can we do to prevent or control CKD?
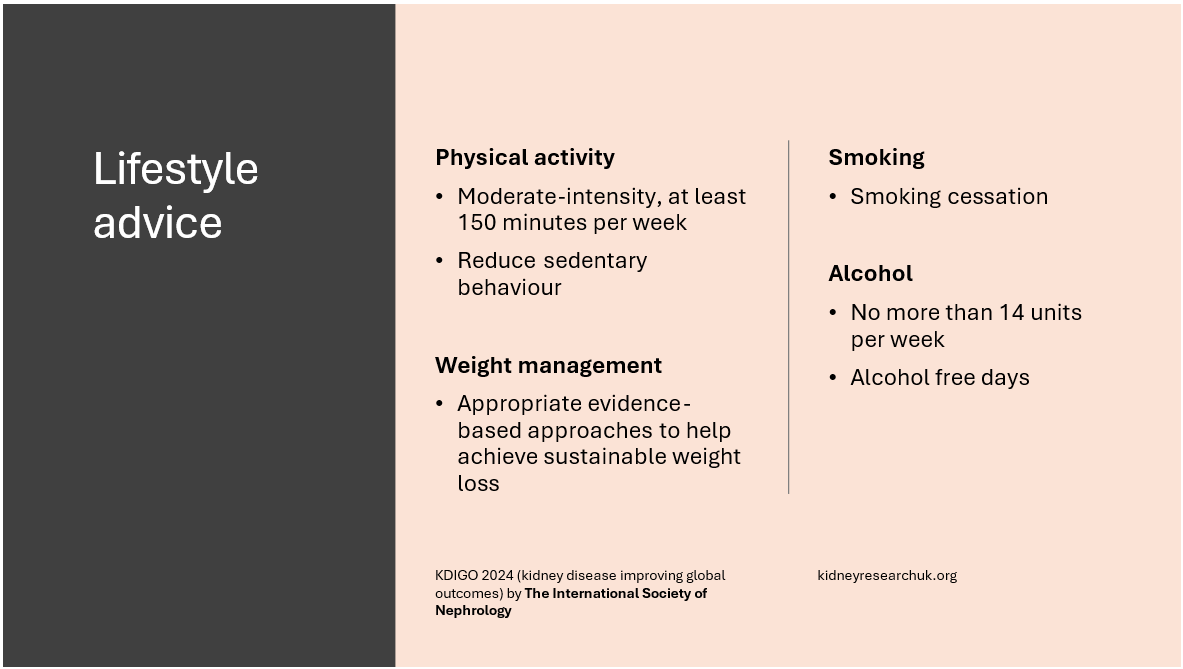
We should ideally get at least 150 minutes of exercise per week at moderate-intensity, or to a level compatible with your cardiovascular and physical tolerance. Recommendations for physical activity should consider age, ethnic background, presence of other comorbidities, and access to resources.
Avoiding sedentary behaviour is key! How long are you sat at your desk, lying on the sofa watching TV, generally sitting? If we can break this behaviour up it all counts. For example, moving your legs and arms for a few minutes when sat at your desk, or getting up for a cuppa whilst the TV ads are on and doing some gentle dancing whilst the kettle is boiling.
Smoking – its advised people with diabetes and CKD who use tobacco to quit using tobacco products to reduce the risk of associated premature mortality from cardiovascular disease, as well as risk of respiratory diseases and cancer.
Smoking can
- Increase risk of developing some kidney cancers
- Damages blood vessels leading to poor blood flow to kidneys
- Causes or advances diabetic kidney disease
- Leads to surges in blood pressure
Diet
People living with diabetes and CKD should consume an individualized diet looking at the below factors …
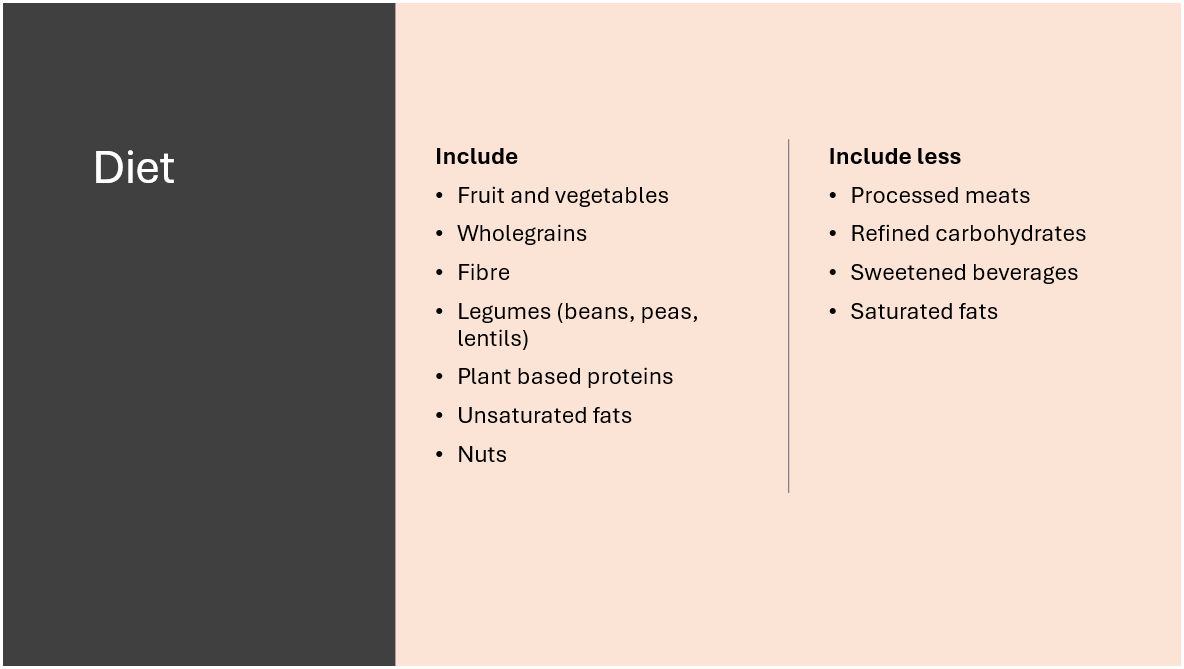
The number of randomised control trails (RCTs) analysing the effects of diet amongst people with diabetes and CKD is small. Most RCTs have a limited number of participants. Application of large, multicentre studies and their results is needed in the context of diabetes, CKD, and diet.
The benefit of consuming fewer refined and processed foods in the general population is well-established, and hence why it's reasonable to apply to those with diabetes and CKD.
Nutrition therapy can decrease HbA1c levels similar to, or better than, those obtained with glucose-lowering medications (in type 2 diabetes). Simple advice such as increasing your intake of non-starchy vegetables, decreasing intake of added sugars and refined grains, and increasing intake of whole foods over highly processed foods can be implemented for most people across wide geographic and economic strata.

Ultra processed foods such as sugar-sweetened beverages, fast foods, frozen meals, and pastries are generally high in salt, sugar, and/or fat, and low in nutritional value. A plant-based diet is rich in anti-inflammatory nutrients, fibre, and phytochemicals. This has been shown to reduce proteinuria and decrease metabolic acidosis. The probiotic nature of plant-based foods may also support the microbiome and reduce inflammation and intestinal production of uremic toxins.
A recent systematic review evaluated the association of dietary patterns and kidney-related outcomes. Dietary patterns that include more plant-based unprocessed protein have been demonstrated, to slow the trajectory of eGFR decline, reduce the risk of kidney failure, reduce risk of mortality, and improve quality of life.
Why are Omega 3 fats good for health?

There has been lots of research into omega 3 fats and oily fish and how they can improve heart health.
In countries where people eat more oily fish, such as in the Mediterranean, Greenland and Japan, fewer people have heart disease compared to countries where people eat very little oily fish, such as the UK.
The Omega 3 fats (EPA and DHA) can help protect the heart and blood vessels from disease: They can help:
- lower triglycerides
- improve circulation
- prevent blood clots
- lower blood pressure
- keep the rhythm of your heart steady
Research suggests omega 3 has beneficial effects for oxidative stress, inflammation and lipid levels. We know conditions like diabetes and CKD are pro-inflammatory, so this is good news.
If you have CKD causes by IgA nephrology (autoimmune conditions which affect the kidneys) omega 3 is often recommended as it has shown to reduce inflammation and thus slow down progression in CKD.
The recommended amount per week is 140g of oily fish eg salmon, mackerel, swordfish. Although renal dietitians may recommend upto 2-3 portions per week for some patients.
Salt
High salt intake raises blood pressure and increases the risk of stroke, cardiovascular disease, and overall mortality.
For those living with CKD, it is recommended we have 5g or less per day. 5g or less per day can be difficult, due to the amount of added salt in processed and ultra processed foods. 6g or less is recommended for general public. The average UK adult has 8g per day, however this may not be that surprising when common foods contain high levels of salt:
2 x average slices of bread contains 0.8g salt
1 x bagel 0.5g salt
Instant noodle pot 2.22g salt
Individual ready meal (spaghetti Bolognese) 1.93g salt
1 shop bought pepperoni pizza 2.9g salt
The other obvious way of reducing salt is not adding it at the cooking stage or at the table. Items such as stock cubes, gravy granules, soy sauce, fish sauce, capers, and olives can all contribute.
Making use of lemon, paprika, chilli, pepper, lime zest, vinegar, cumin etc are all great ways of adding flavour instead of salt.
British food culture

If you search British way of eating on the internet, things like fish and chips, English breakfast, and bangers and mash appear regularly. The above items contain fat, salt, and some sugar. No vegetables are in sight apart from the Sunday roast. Fun or ‘sole foods’ like these are fine to include occasionally, however health could be affected if foods like the ones listed above were an everyday thing.
Many of the above foods fall into the processed or ultra processed food (UPF) category. For more information about ultra processed foods, take a look at Ultra processed foods and type 2 diabetes (spoonernutrition.co.uk)
There is no definitive evidence about the health impact of eating ultra-processed food. However, a recent study in the British Medical Journal- based on information from 9.9 million people worldwide – linked them to:
- a higher risk of death from cardiovascular illnesses
- obesity
- type 2 diabetes
- sleep problems
- anxiety and depression
The study could not prove it was the processing of food that caused the illnesses, or simply the fact that most of them are high in fat, sugar and salt. These are a known cause of weight gain, type 2 diabetes, heart disease and some cancers.
Consumption of UPF may be an indicator of other unhealthy dietary patterns and lifestyle behaviours. Diets high in UPF are often energy dense, high in saturated fat, salt or free sugars, high in processed meat, and/or low in fruit and vegetables and fibre.

In more advanced stages of CKD further dietary changes may be required, such as reducing the amount of phosphate or potassium in the diet. Hyperphosphatemia may occurs in CKD stage 4-5 and is associated with mineral bone disease. Properly functioning kidneys remove extra phosphate that ends up in the body, but with CKD, the kidneys can’t remove the phosphate, causing it to build up.
Phosphate is regularly found in meat, fish, diary and very commonly found in food additives in UPFs, eg E338 (phosphoric acid) E339 (sodium phosphates) and E340 (potassium phosphates). Phosphate containing food additives are often in cakes, biscuits, processed meats, spreadable and slices processed cheese, dried powdered sauces or soups. They often have 90-100% bioavailability and are readily absorbed into the body.
So, as you can see UPF pose an even higher risk for more advanced levels of CKD.

Send us a message
Contact Us
Thank you for contacting us.
We will get back to you as soon as possible.
Oops, there was an error sending your message.
Please try again later.
Spooner Nutrition








